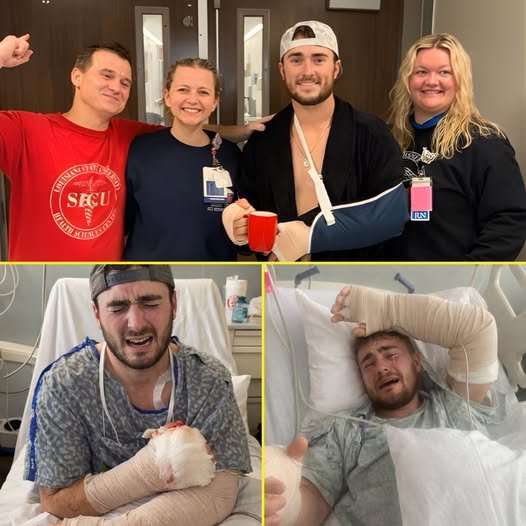
The language has shifted.
No one is speaking in long-term projections right now. The focus is immediate. Measured. Tactical.
Hunter may face 2–3 additional surgeries in the coming days — not because the team is reacting blindly, but because complex electrical injuries often require staged surgical management.
And that distinction matters.
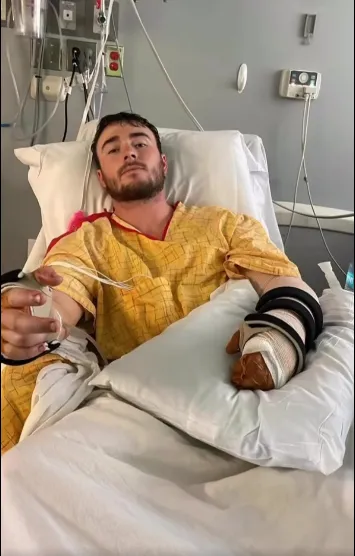
⚡ Why Multiple Surgeries Happen in Waves
Electrical trauma doesn’t always reveal its full extent at once. Damaged tissue can declare itself over time. Surgeons often have to:
- Remove clearly nonviable tissue
- Preserve borderline areas to see if blood flow improves
- Reassess circulation and swelling
- Return to the OR if deeper compromise becomes clear
It’s not that damage is “spreading” like an infection unchecked.
It’s that the body is still demarcating what can survive and what cannot.
That process unfolds in hours and days — not months.
🩸 The Surgical Balancing Act
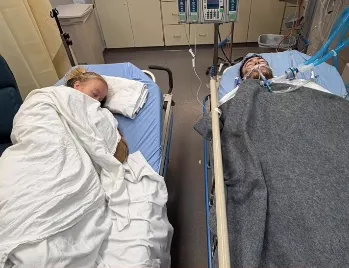
The fear families feel is real because the timing is delicate.
Intervene too late, and nonviable tissue can threaten surrounding structures.
Intervene too early, and you may sacrifice tissue that might have recovered.
This is not guesswork — it’s calculated medicine guided by:
- Tissue color and capillary refill
- Doppler vascular flow
- Inflammatory markers
- Compartment pressure
- Response to prior debridement
Each procedure is designed to protect long-term function, not gamble it.
🏥 How Many Surgeries Can a Body Endure?
Medically, the human body can tolerate multiple operations — especially when they are controlled, staged, and carefully monitored.
What determines endurance isn’t just the number of surgeries, but:
- Hemodynamic stability
- Nutritional status
- Infection control
- Pain management
- Organ function
- Psychological resilience
If those systems remain supported, repeated procedures — while exhausting — are survivable.
The emotional toll is often heavier than the physiological one.
🔬 Is the Damage Truly “Spreading”?
With electrical injuries, what looks like aggressive spread is often delayed declaration.
The current may have injured deep tissue at the moment of contact. The surface can look stable while muscle, fascia, or microvasculature declare compromise later.
It’s not new damage forming overnight.
It’s original damage becoming visible.
That’s why these cases feel relentless.
🛡️ This Isn’t Standard — But It Isn’t Hopeless
You’re right: this isn’t a smooth, linear recovery.
It’s surgical survival mode.
But multiple planned interventions are often a sign that:
- There is still viable tissue worth saving
- Circulation is present
- The limb remains salvageable
- The team believes function can be preserved

If the situation were beyond salvage, the strategy would look very different.
Right now, the approach suggests protection — not surrender.
💔 Why It Feels So Heavy
For the family, every trip to the OR feels like rolling dice with the future.
Will this one stabilize things?
Will this one take more than expected?
Will this be the last — or the beginning of another wave?
That uncertainty is brutal.
But the pace of surgery doesn’t automatically mean the body is failing.
It means the team is actively preventing failure.
📌 The Real Question
Not “How many surgeries before the cost is too high?”
But:
Is he stable enough to keep fighting?
Is circulation present?
Are surgeons still pursuing function?
If those answers remain yes, then the strategy is still preservation.
Recovery in severe electrical trauma is rarely elegant.
It’s incremental.
It’s surgical.
It’s exhausting.
But it’s not the same as collapse.
Right now, the clock is loud — but it hasn’t run out.
And the fact that surgeons are still operating to save tissue means there is still tissue worth saving.