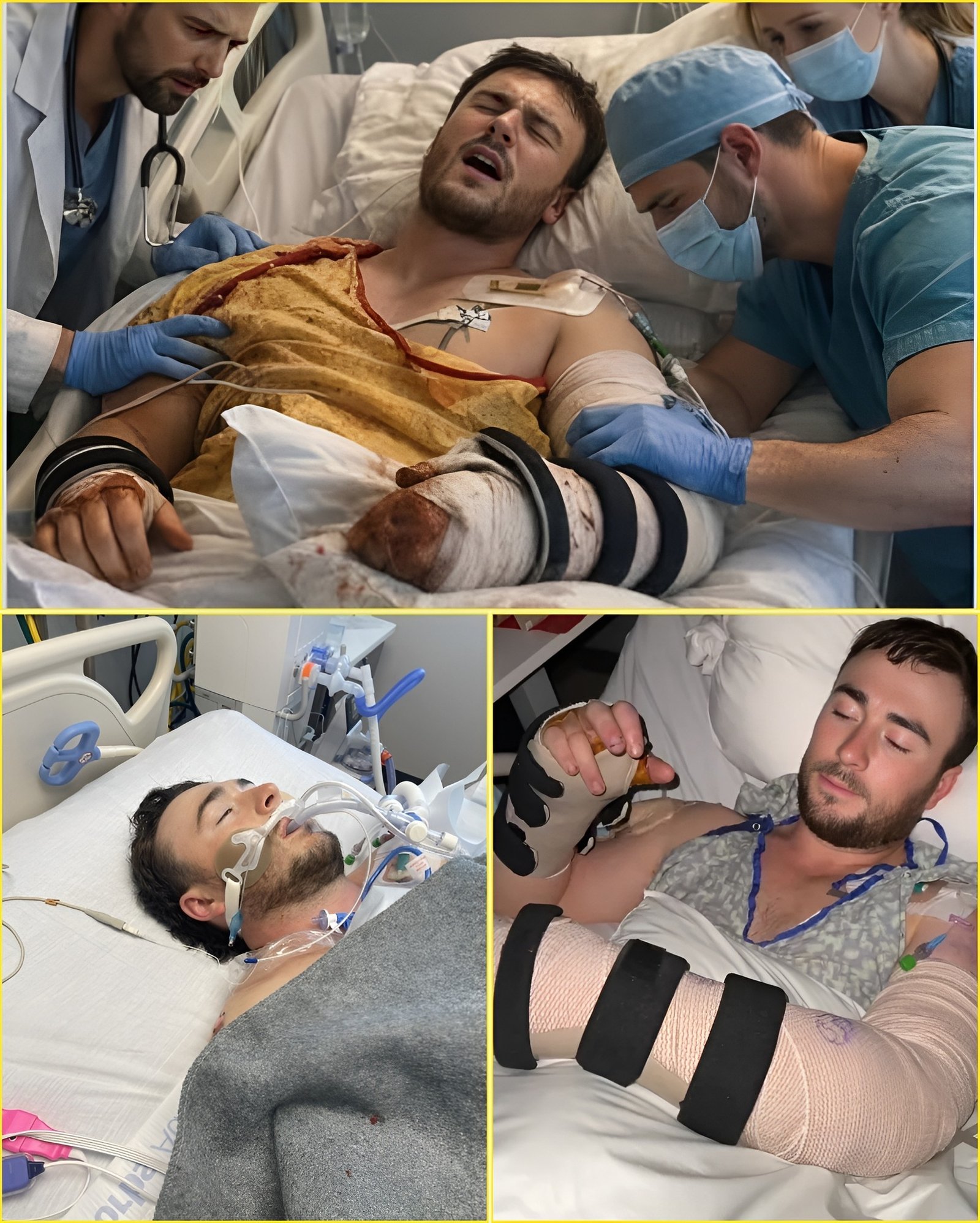
The room didn’t erupt in chaos. It tightened.
What had been described as fragile but steady recovery has shifted into something far more intense.
Hunter is now under the highest level of ICU monitoring after doctors identified erosion affecting a blood vessel near a previous surgical site — a development that instantly escalated concern.
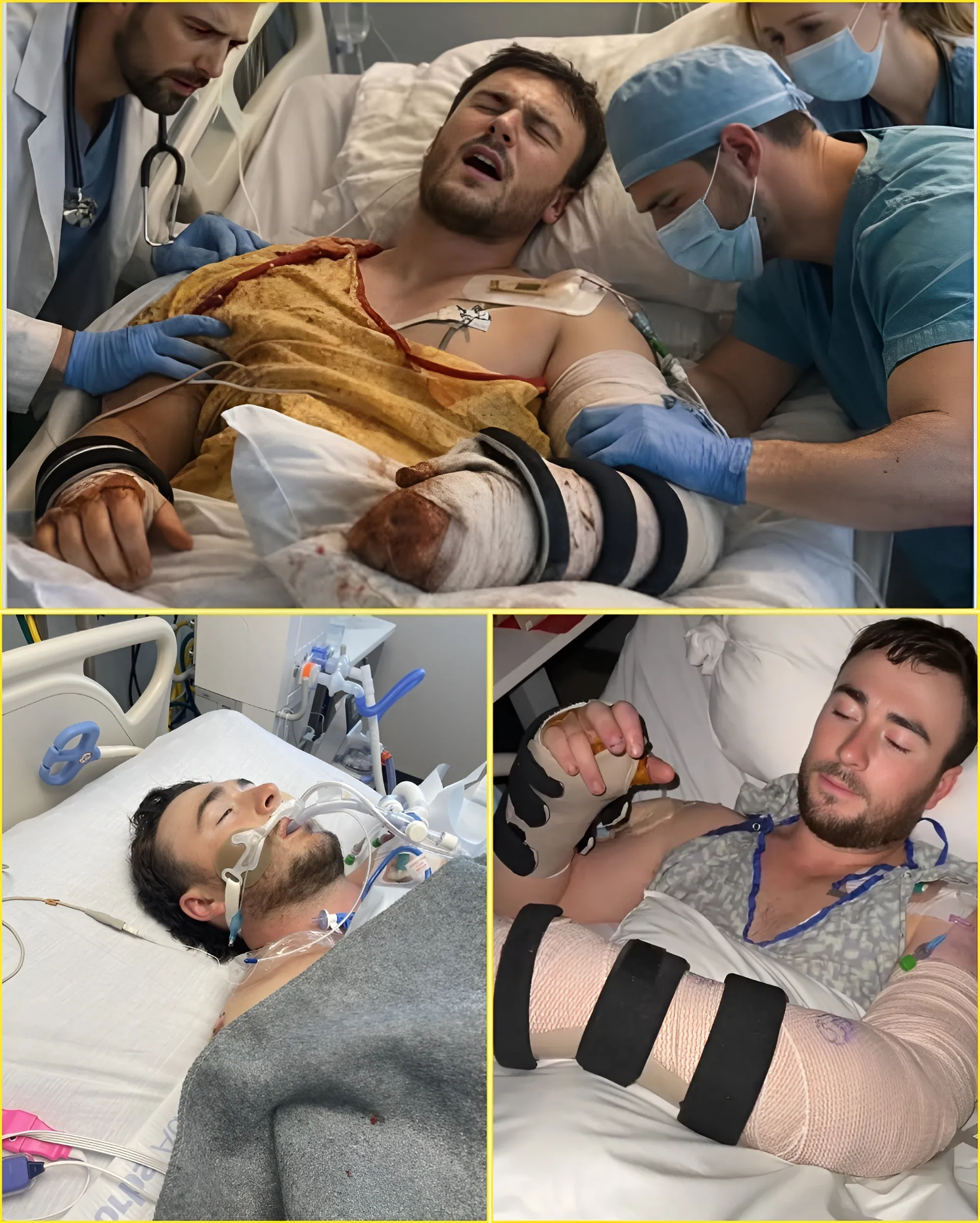
And in electrical trauma cases like his, vascular erosion is not a minor complication.
It’s a red alert.
When the Hidden Damage Surfaces
High-voltage electrical injuries don’t behave like typical trauma.
The initial burns are only part of the story. The real destruction often travels deep — through muscle layers, nerve pathways, and blood vessel walls. Even when tissue appears stable at first, damage can evolve over time.
That’s what makes this moment so serious.
When a vessel wall weakens or erodes, the risk is not gradual decline.
It’s rupture.
And rupture means rapid, potentially massive bleeding.
Minutes matter.
That’s why the tone inside Hunter’s ICU room changed immediately.
The Shift to Maximum Surveillance
Hunter is now under continuous, high-level ICU observation.
Every heartbeat is tracked in real time.
Blood pressure is monitored beat-by-beat.
Hemoglobin levels are being checked frequently to detect even subtle drops that could indicate internal bleeding.
Circulation markers and limb perfusion are under constant review.
Access to his room has been limited.
Not as symbolism.
As strategy.

Reducing foot traffic lowers infection risk and eliminates distractions during an unstable window. Electrical trauma patients are particularly vulnerable because repeated surgeries and damaged tissue weaken immune defenses.
In vascular cases, precision is everything.
Why Stability Isn’t Enough
To someone outside the ICU, the escalation might feel alarming.
If he looks stable, why the lockdown-level vigilance?
Because vascular erosion is unpredictable.
A patient can appear stable — normal vitals, controlled pain, steady labs — and then deteriorate rapidly if a weakened vessel fails.
That’s the danger.
ICU-level observation allows physicians to detect the smallest deviation immediately:
• A subtle blood pressure dip
• A rapid heart rate change
• A hemoglobin drop before symptoms appear
• Swelling or expanding hematoma near the surgical site
• Changes in limb temperature or coloration
Early detection is the only advantage in scenarios like this.
They are not waiting for visible crisis.
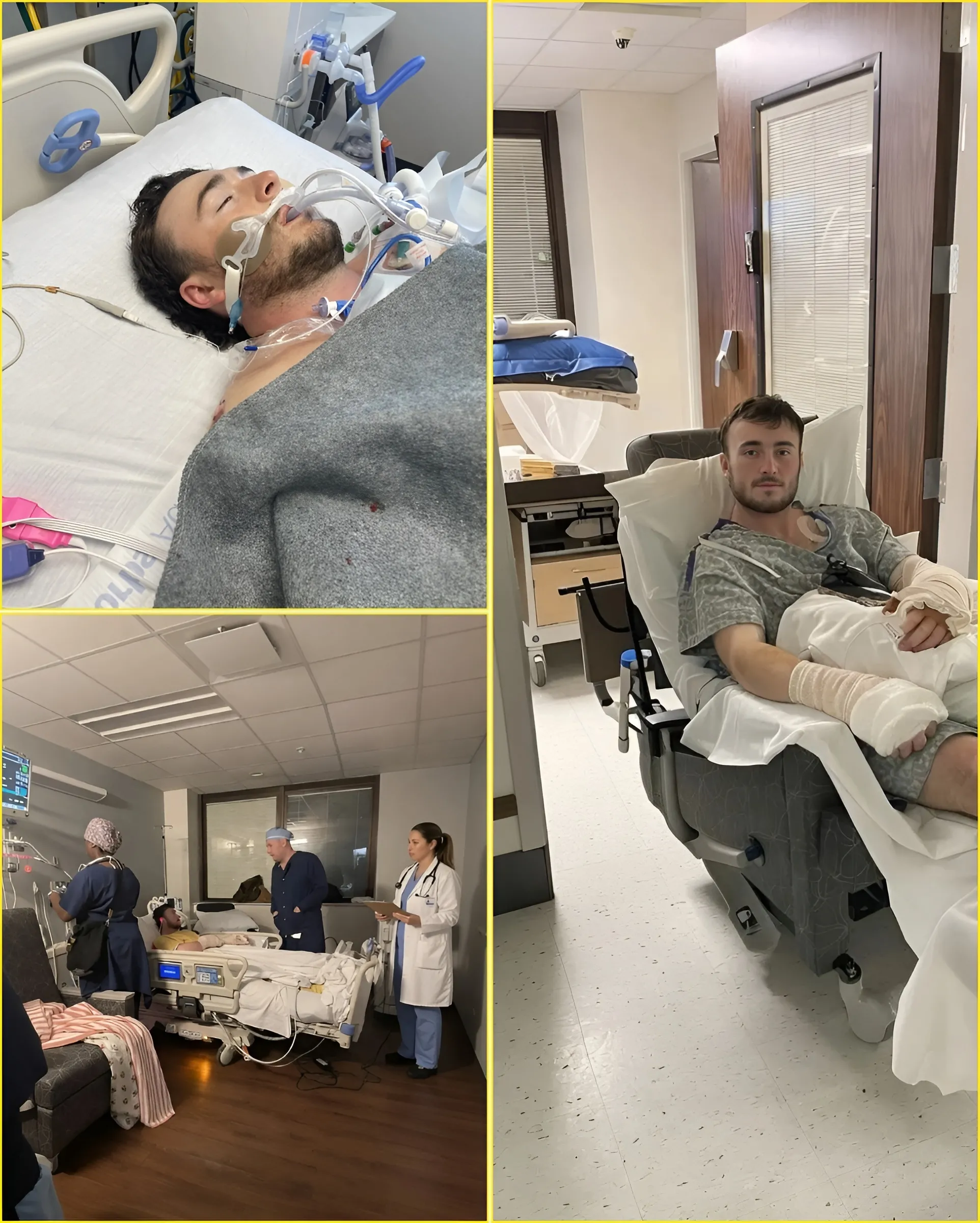
They are hunting for the earliest signal of one.
Behind the Scenes: Prepared, Not Panicked
Publicly, doctors are not using catastrophic language.
Privately, contingency planning is fully activated.
Emergency blood products are cross-matched and ready.
Operating room access can be mobilized without delay.
Surgical teams are aware and on standby.
Care plans are mapped hour by hour.
This does not mean rupture is inevitable.
It means they refuse to be surprised.
The ICU mindset right now is dual-track:
Hope for stability.
Prepare for intervention.
The Critical Window
The next 12 to 24 hours are pivotal.
If vascular integrity holds — if hemoglobin remains stable, blood pressure steady, and no perfusion shifts appear — monitoring may gradually ease.

If thresholds are crossed, intervention will be immediate.
And those thresholds are not emotional.
They are numerical.
Critical care teams rely on precise data points to determine when observation ends and action begins.
For Hunter, those markers are clearly defined.
Everyone on that unit knows them.
The Emotional Weight
Hunter’s family remains close, though visits are carefully managed.
Communication continues steadily. Physicians are explaining each lab value, each precaution, each change in monitoring intensity.
The goal is clear:
Prevent rupture.
Protect circulation.
Buy time for the vessel to stabilize and repair to hold.
This phase is not about dramatic procedures.
It’s about guarding against catastrophe.
Electrical Trauma: The Unpredictable Opponent
Electrical injuries are among the most complex in trauma medicine because damage unfolds in layers.
Tissue that survives one surgery can weaken days later.
Vessels stressed by heat and current can deteriorate even after careful repair.
Inflammation can shift suddenly.
Escalation in monitoring does not mean failure.
It reflects the known behavior of this kind of injury.
Hunter is under intense surveillance precisely because his team intends to intercept complications before they spiral.
Where Things Stand
At this hour:
• Vitals are stable.
• Blood products are prepared but not deployed.
• Surgical teams are ready but not activated.
• ICU monitoring remains at maximum intensity.
The room is quiet.
But alert.
And while the risk is real, so is the vigilance surrounding him.
In complex trauma care, survival often depends less on avoiding complications — and more on detecting them early enough to act.
Right now, Hunter’s greatest protection is not calm.
It is constant watchfulness.
Updates will follow as doctors continue evaluating the vascular repair and monitoring for any sign that would require immediate surgical response.