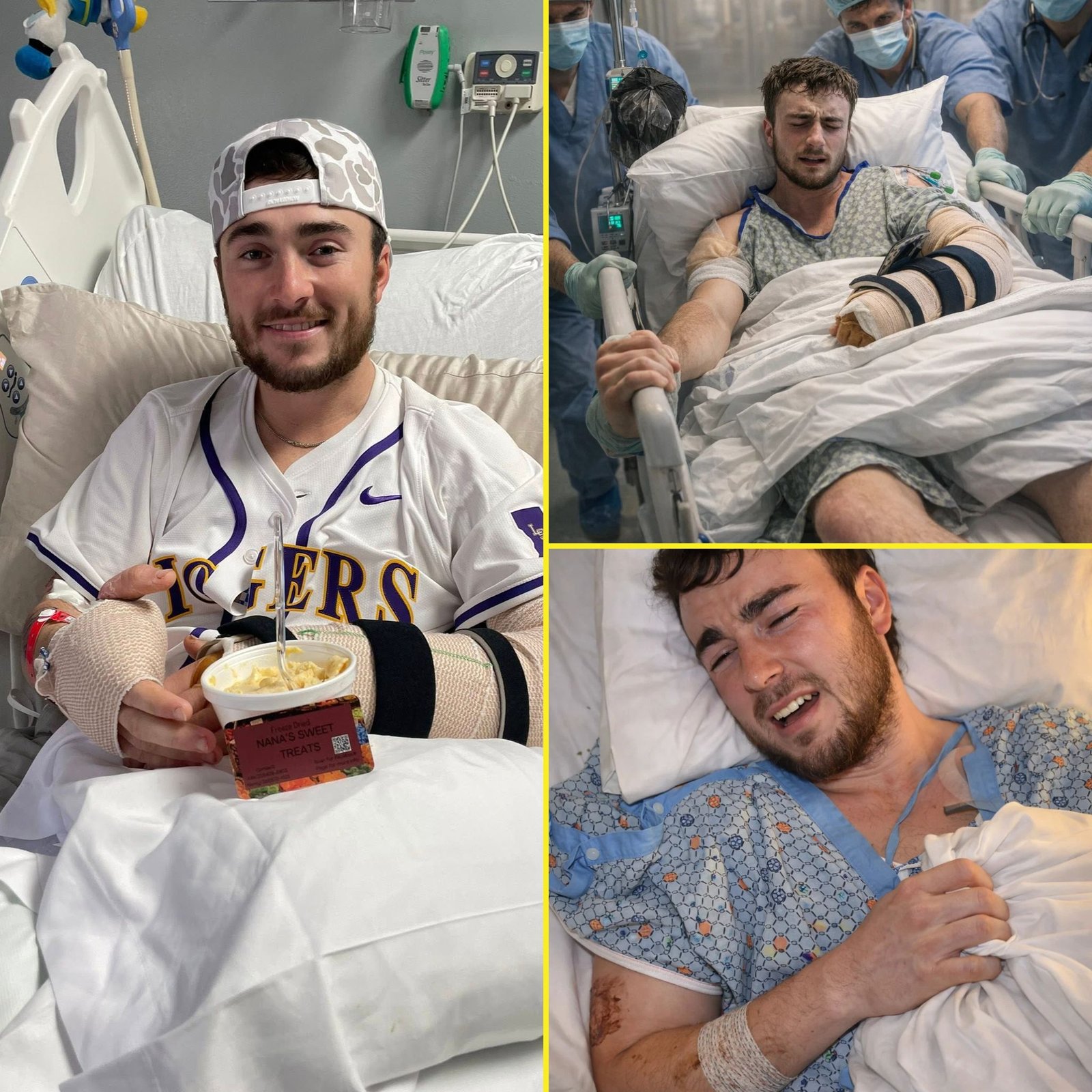
As Hunter Alexander was wheeled past his family, the only steady sound was the rhythmic beep of monitors tracking a body that has already endured more than most ever will. Hands reached out gently as he passed. Fingers brushed against blankets. Prayers weren’t spoken loudly — they barely made it above a whisper.
Because tomorrow isn’t routine.
In just 24 hours, Hunter will undergo a critical debridement procedure — one doctors say could significantly influence the direction of his recovery. The term itself sounds clinical, almost sterile. But for the family, it carries weight far beyond medical vocabulary.
Debridement means removing damaged or dead tissue to prevent infection and allow healthy healing. In trauma cases, it’s often necessary. Sometimes lifesaving. But how much tissue must be removed can shift the entire trajectory of rehabilitation.
That’s why the phrase now circulating among loved ones is specific and urgent:
“Pray the debridement is minimal.”
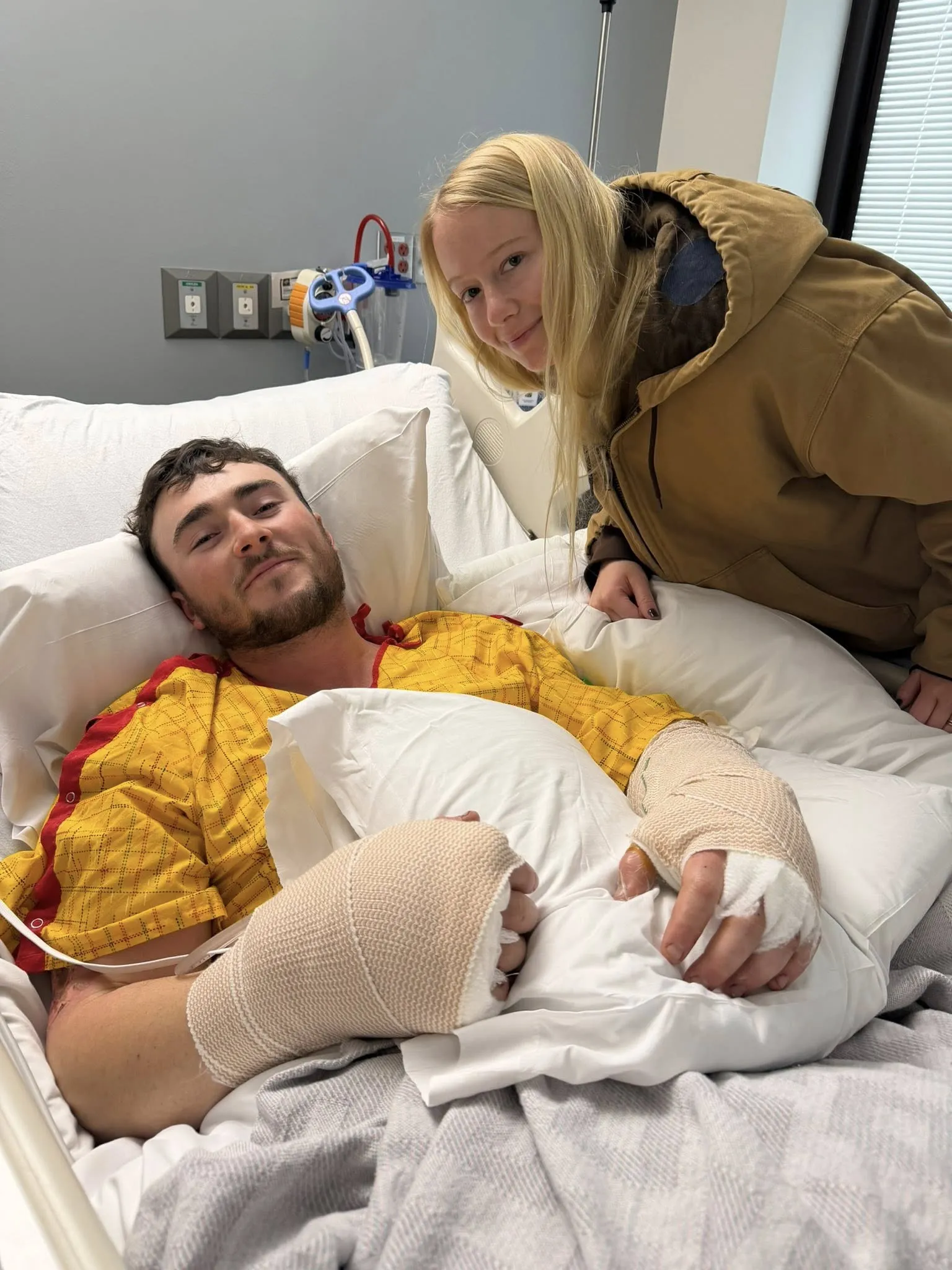
This isn’t about drama. It’s about margin.
What began as a sudden medical emergency has evolved into a race against infection, inflammation, and time. Surgeons are preparing with precision, aware that each millimeter of compromised tissue tells a story about what the body has endured — and what it can still sustain.
Medical teams are clear: this procedure is essential. But they are also realistic. The extent of tissue removal won’t be fully known until they’re inside the surgical field. Imaging offers guidance. Experience offers prediction. But only direct examination reveals certainty.
And certainty is something this family has not had much of lately.
In earlier stages, surgeries focused on stabilization — preserving circulation, protecting nerves, preventing systemic complications. Now the focus narrows to quality and viability. It’s not just about survival. It’s about what kind of healing is possible.
Each update has carried cautious optimism. Yet each step forward seems paired with a reminder that setbacks remain possible. Infection is patient. Healing is unpredictable. And tissue that looks stable externally can reveal deeper damage when examined closely.
That’s why tomorrow feels like more than “another procedure.”
It feels like a pivot point.
Will surgeons find mostly healthy tissue, requiring only limited removal and setting the stage for grafting and reconstruction? Or will the damage run deeper, demanding more aggressive intervention and extending the timeline?
No one is predicting the worst.
But no one is dismissing the stakes.
Family members admit the waiting is the hardest part. Once surgery begins, there’s nothing left to do but sit under fluorescent lights and count the passing hours. Phones stay close. Conversations stay short. Hope becomes focused — not broad and abstract, but narrow and targeted.
Minimal removal. Strong circulation. Clean margins.
Doctors, for their part, are balancing preparedness with restraint. They will remove what must be removed. No more. No less. The goal is preservation — but preservation must be safe.
And that balance is what makes debridement such a defining moment in complex recoveries.
Supporters continue to flood social media with messages of faith and encouragement. The phrase “pray the debridement is minimal” has spread quickly, reflecting both fear and determination. It’s a plea rooted in understanding: every piece of tissue spared may mean stronger function later. Shorter rehabilitation. Fewer complications.
Tomorrow’s surgery will not end the journey.

But it may clarify it.
In hospital corridors tonight, the air feels thinner. Every sound sharper. Every hour slower. Hunter’s family knows the medical team is capable. They know procedures like this are part of the process.
Still, knowing that doesn’t quiet the question echoing beneath everything else:
When the surgeons step out tomorrow, will they be describing a turning point toward healing — or a longer road than anyone is ready to face?
For now, the monitors continue their steady rhythm.
And the prayers remain specific.