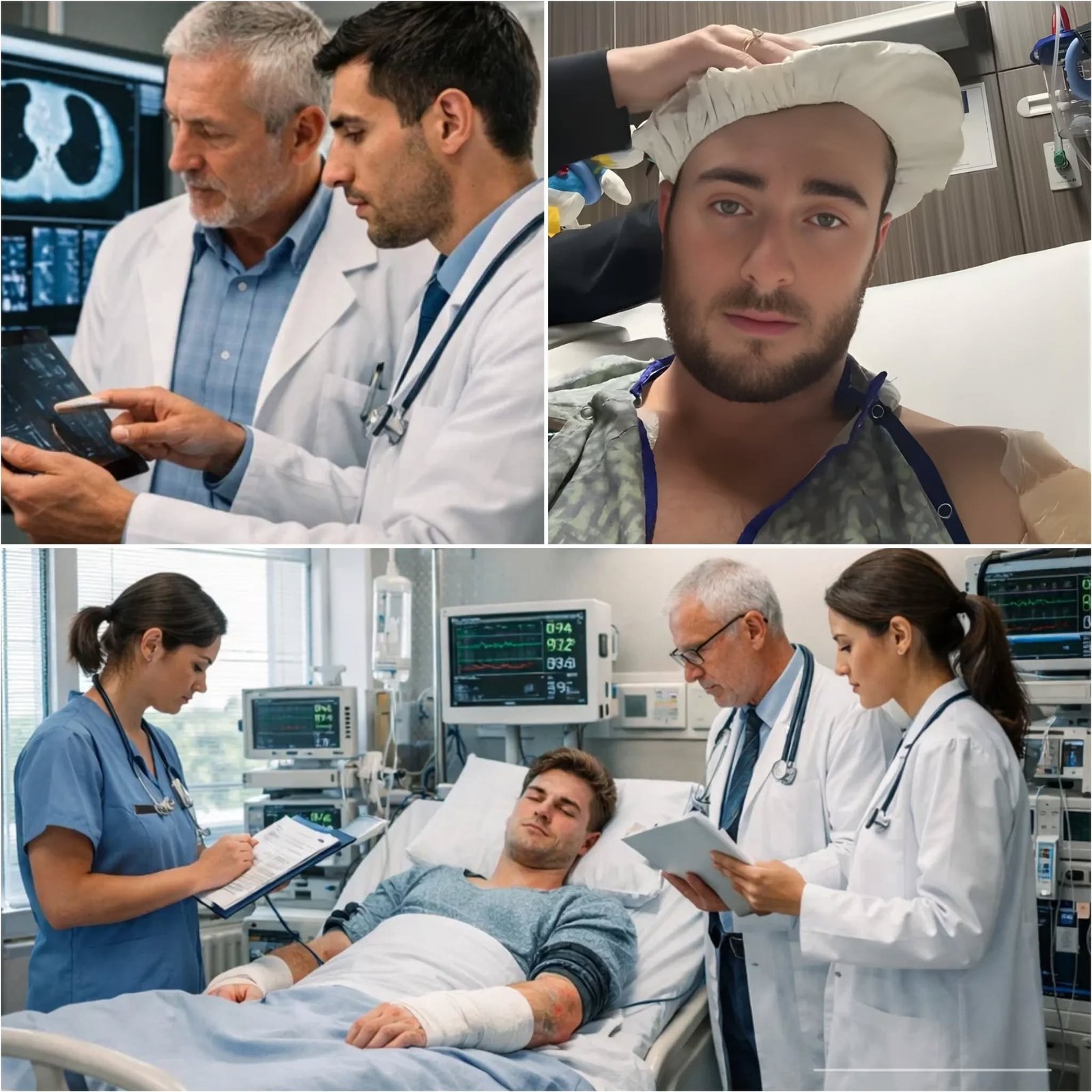
The surgery was meant to stabilize the situation.
Doctors had moved forward with a fasciotomy, a procedure used to relieve
dangerous pressure inside muscle compartments, along with aggressive debridement to remove damaged tissue.
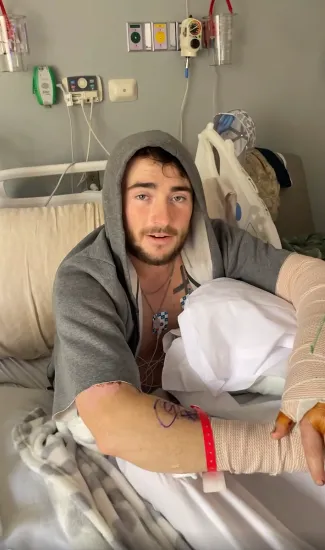
The goal was clear: protect circulation, stop the spread of injury, and give healthy tissue the best chance to survive.
It was urgent — but it was supposed to help.
Then Hunter’s father delivered the update.
And the tone changed instantly.
According to him, the condition on the left side of Hunter’s body was “profoundly worse.”
Those two words landed heavily.
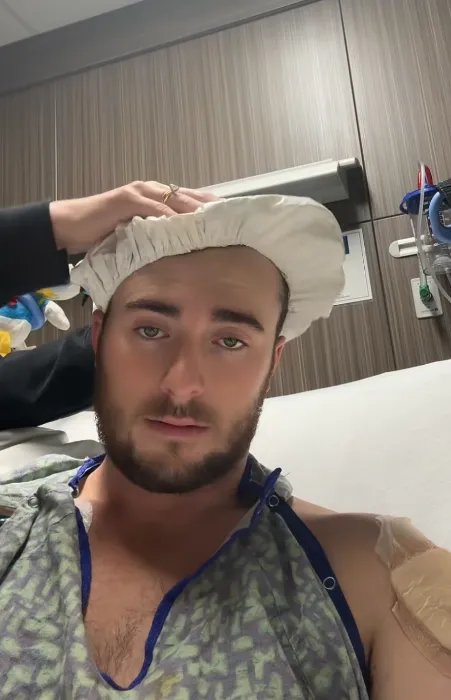
Because “profoundly worse” doesn’t mean minor swelling or routine surgical cleanup.
It suggests damage deeper than doctors had initially seen — damage that only became fully visible once surgeons were inside the operating field.
Inside the ICU, the atmosphere shifted.
Nurses adjusted monitoring equipment with renewed urgency. Doctors gathered in tight discussions.
Voices dropped to quiet, focused tones as teams began reassessing the next steps.
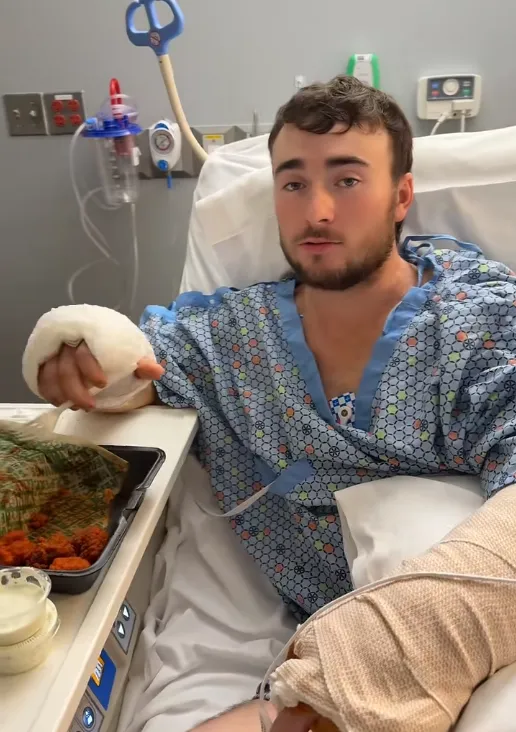
What had been a procedure meant to relieve pressure had suddenly revealed a much more serious battle beneath the surface.
A fasciotomy is not a small intervention. It is performed when swelling inside muscle compartments becomes
so severe that it threatens to cut off blood flow entirely — a condition known as compartment syndrome.
If untreated, it can lead to permanent tissue damage.
That’s why surgeons also performed debridement,

removing tissue that could no longer survive in order to prevent infection and allow healthier areas to heal.
But during the operation, doctors discovered something that had not been fully visible before surgery began.
The damage on Hunter’s left side extended further than early scans had suggested.
In trauma medicine, this can happen more often than people realize.
Electrical injuries and vascular complications can destroy tissue deep beneath the skin while leaving the surface deceptively stable.

Sometimes the full extent only becomes clear when surgeons physically examine the area during surgery.
For Hunter’s family, the realization was devastating.
They had prepared themselves for difficult news —
but the words “profoundly worse” carried a weight that few were ready for.
Now the ICU has shifted into an even higher level of vigilance.

Doctors are closely monitoring:
• blood circulation through the injured areas
• nerve response and neurological signals
• infection markers in vulnerable tissue
• overall organ stability after surgery
Every reading matters.
Every hour matters.

In severe trauma cases, once deeper damage is revealed, the focus becomes containment and preservation
— stopping further deterioration while protecting any tissue that can still recover.
No one is declaring defeat.
Doctors continue working.
Treatments continue.
Monitoring remains constant.

But one thing has changed.
The situation is now being understood in its full severity.
For the family, the waiting has become heavier.
For the medical team, the mission is clear: protect circulation, stop the spread of damage, and stabilize Hunter’s condition.
And for the thousands following his journey, the latest update is a painful reminder of how unpredictable trauma recovery can be.

The surgery meant to relieve pressure revealed a deeper crisis.
Now the fight has entered a more critical phase.
And every hour moving forward will matter.