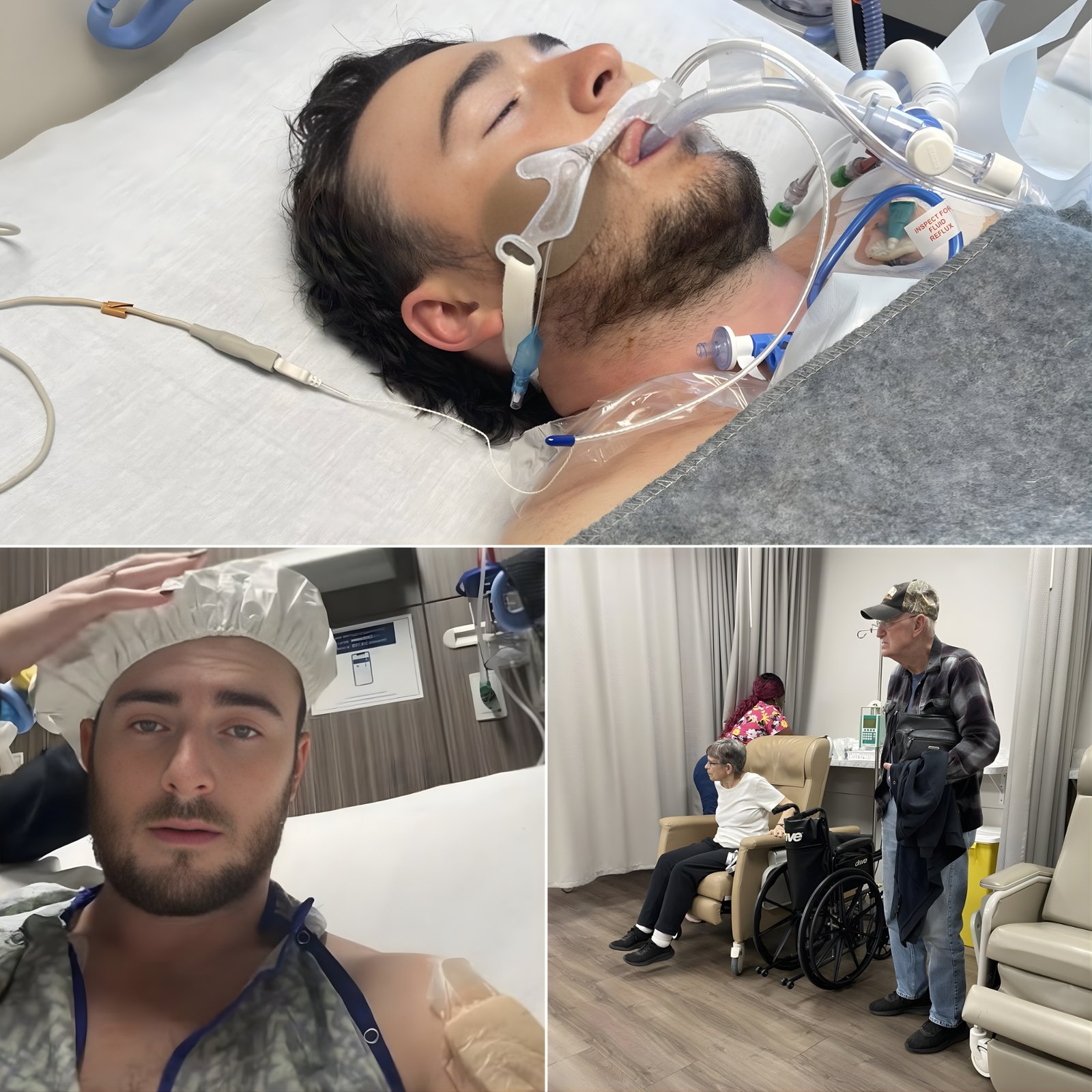
As Hunter prepares for tomorrow morning’s operation, the atmosphere in the trauma unit has shifted from reactive urgency to deliberate focus.
This procedure — a planned surgical debridement — is not sudden. It is strategic.
And while it carries weight, it is also a standard and necessary part of managing severe electrical injuries.
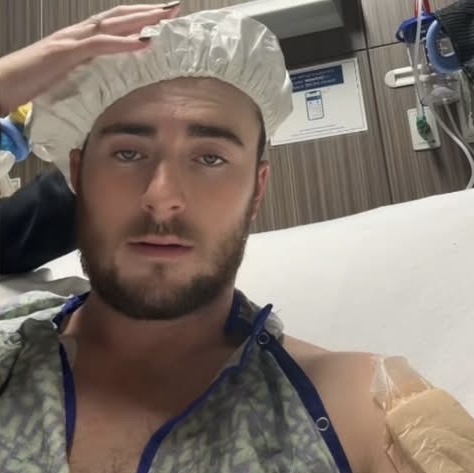
The question is not whether surgeons will operate.
It’s how much non-viable tissue they will find — and how much healthy structure can be preserved.
What Debridement Actually Means
Debridement is the surgical removal of dead (necrotic) tissue.
In high-voltage electrical injuries, tissue damage can extend far beneath the skin.
Unlike flame burns, electrical current travels through muscle and vascular pathways, sometimes causing internal destruction that evolves over days.
If dead tissue is not removed:
- Infection risk rises sharply
- Sepsis becomes possible
- Healing stalls
- Surrounding viable tissue becomes threatened
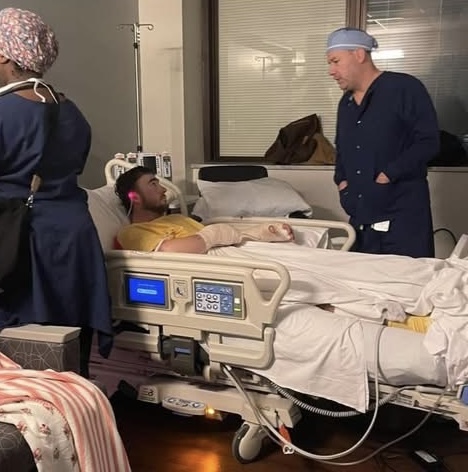
Debridement is not a punishment or a sign of failure.
It is a protective intervention.
The goal is always the same:
Remove what cannot survive.
Preserve what can.
Why Electrical Injuries Complicate Timing
Electrical trauma is progressive.
Damage does not always fully declare itself immediately.
Surgeons sometimes perform staged debridements — returning to reassess tissue viability as swelling decreases and blood flow patterns clarify.
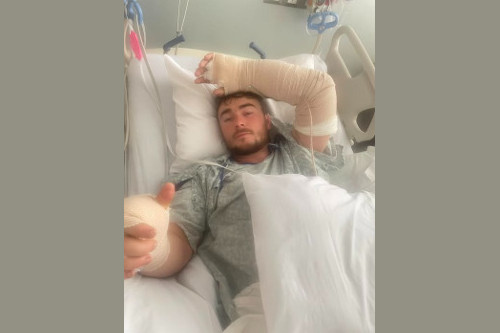
A muscle that appears questionable early on may recover.
A section that appears stable may later declare itself non-viable.
Tomorrow’s surgery is about clarity.
It allows surgeons to directly visualize tissue, assess blood supply, and make evidence-based decisions rather than relying solely on imaging or surface appearance.
The Balance Surgeons Must Strike
The surgical team faces a familiar but difficult balance:
- Remove too little → risk infection and systemic spread
- Remove too much → sacrifice potentially recoverable function
This is not guesswork. Surgeons use:

- Color and bleeding response of tissue
- Contractility testing
- Vascular flow assessment
- Intraoperative judgment refined by burn and trauma experience
The objective is always maximal preservation with minimal risk.
It is rarely binary.
It is careful, layered decision-making.
Why Tonight Feels Heavy
For families, debridement sounds like subtraction.
For surgeons, it is stabilization.
The emotional tension comes from uncertainty — not inevitability.
Until tissue is directly assessed under surgical light, no one can predict the exact extent of removal required.
That uncertainty is what weighs on the room tonight.
Not drama.
Not collapse.
But anticipation.
What Doctors Are Watching Before Surgery
Overnight, medical teams are monitoring:
- Circulatory stability
- Temperature trends
- Inflammatory markers
- Hydration and metabolic balance
- Tissue perfusion

The body is being optimized for surgery — fluids balanced, antibiotics adjusted, anesthesia plans reviewed.
Preparation matters. Stability going in improves outcomes coming out.
What “Minimal Debridement” Means Clinically
When families say they are hoping for “minimal debridement,” medically that translates to:
- Clear demarcation between viable and non-viable tissue
- Limited necrosis progression
- Preserved vascular channels
- Strong bleeding response from muscle edges
It means the injury has stopped advancing.
It means the body has drawn its boundary.