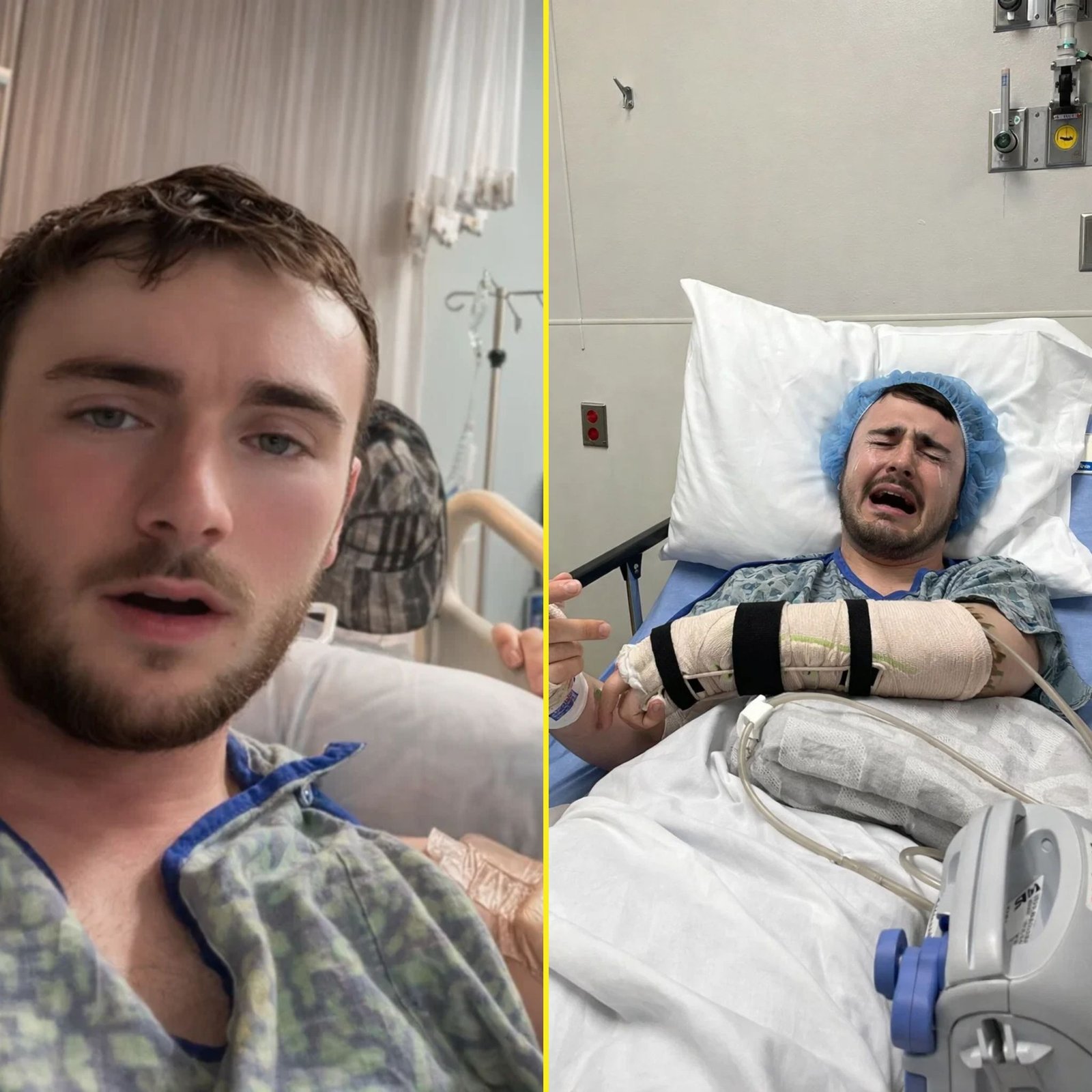
The surgery was supposed to help.
After mounting concerns about swelling and tissue pressure, doctors moved forward with a fasciotomy — a procedure designed to relieve dangerous internal compression — along with aggressive debridement to remove compromised tissue and prevent further spread of damage. It was framed as urgent but necessary. A step to protect circulation. A measure to preserve function.
But when Hunter’s father stepped forward afterward, his voice carried something heavier than cautious relief.
The left side of Hunter’s body, he said, was “profoundly worse.”
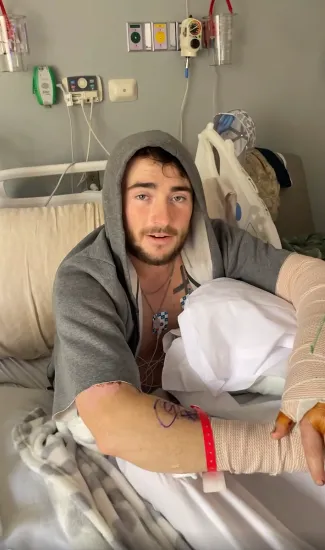
Those two words didn’t just update the situation — they detonated it.
Because “profoundly worse” doesn’t describe mild inflammation. It doesn’t suggest routine surgical cleanup. It signals something deeper. Structural. Potentially escalating.
Inside the ICU, the atmosphere shifted almost immediately.
Nurses adjusted monitors with sharper focus. Physicians gathered in tighter circles. Conversations dropped in volume but increased in intensity. The room, already heavy with tension from prior complications, began to feel less like a recovery space and more like a frontline response zone.
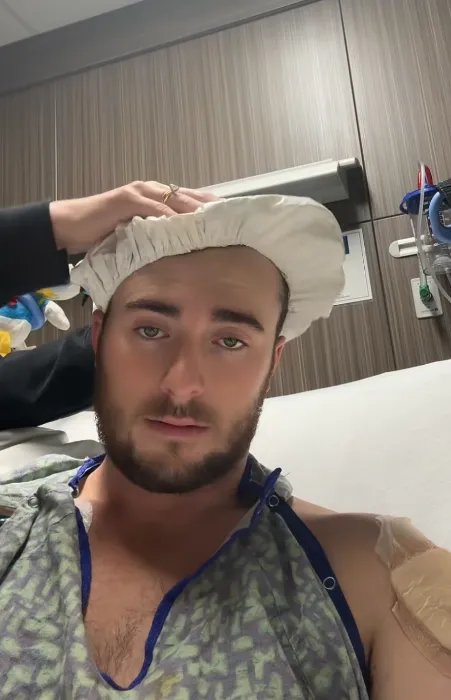
A fasciotomy is not a minor intervention. It’s performed when pressure within muscle compartments becomes so severe that it threatens blood flow and tissue survival — a condition that can lead to permanent damage if not addressed quickly. Debridement, meanwhile, is the removal of tissue that is dead or no longer viable, often to prevent infection from spreading or to give healthy tissue a chance to heal.
The expectation going in was clear: relieve the pressure, remove compromised areas, stabilize the situation.
But what surgeons discovered mid-procedure appears to have exceeded those expectations.
Though official medical details remain measured and controlled, the father’s phrasing — “profoundly worse” — suggests the damage extended beyond what imaging or surface indicators had initially revealed. In complex trauma and vascular-compromised cases, tissue can deteriorate rapidly beneath the surface. Circulatory disruptions, inflammation, or microvascular injury can progress silently before manifesting dramatically once surgically exposed.
If that is what occurred, it explains the sudden tonal shift.
Family members describe being blindsided by the severity. There had been warnings. There had been concerns. But nothing that prepared them for language that stark.
The question now echoing among supporters and observers is painful but persistent:
Why wasn’t the depth of the damage revealed earlier?
Medical reality can offer part of that answer. Surgeons often don’t fully grasp the extent of tissue compromise until they operate. Imaging scans can suggest pressure or irregularity, but they cannot always distinguish between tissue that is struggling and tissue that is unsalvageable. In fast-moving conditions, deterioration can accelerate within hours.
That doesn’t ease the shock. But it may explain the gap between expectation and discovery.
Another layer of tension stems from communication timing. In high-risk surgical environments, doctors frequently wait until procedures are complete before discussing findings with family — especially if the situation evolves mid-operation. Decisions are made in real time. Priorities shift from explanation to action.
Still, the emotional fallout is real.
Supporters describe feeling as though the narrative changed without warning. One moment, the surgery was described as pressure relief. The next, it was a revelation of something much darker.
Complications spreading on one side of the body raise additional concerns: compromised blood supply, nerve involvement, potential systemic inflammatory response. Each possibility carries its own risks and its own urgency.
Inside the ICU, vigilance intensified again.
Post-surgical monitoring has become hyper-focused on circulation markers, neurological response, infection indicators, and organ stability. When damage proves deeper than expected, the window for preventing further cascade narrows. That’s why movements became faster. That’s why voices lowered. That’s why the energy felt charged.
Family members are now grappling with layered fear — not just about what has already been lost, but about what might still be at stake.
In severe cases involving compartment syndrome or extensive tissue compromise, outcomes depend heavily on timing. Early intervention can save function. Delayed recognition can mean irreversible consequences. If the deterioration was more advanced than anticipated, the urgency to stabilize the remaining viable tissue becomes critical.
No one is publicly declaring defeat. Doctors continue working. Interventions continue. Monitoring remains relentless.
But the language has changed.
“Profoundly worse” leaves little room for casual optimism.
And yet, it also reflects transparency from a father who chose blunt honesty over softened reassurances. In moments like these, families often walk a line between protecting hope and confronting reality. His words suggest that shielding the truth no longer felt possible.
The ICU does not resemble surrender.
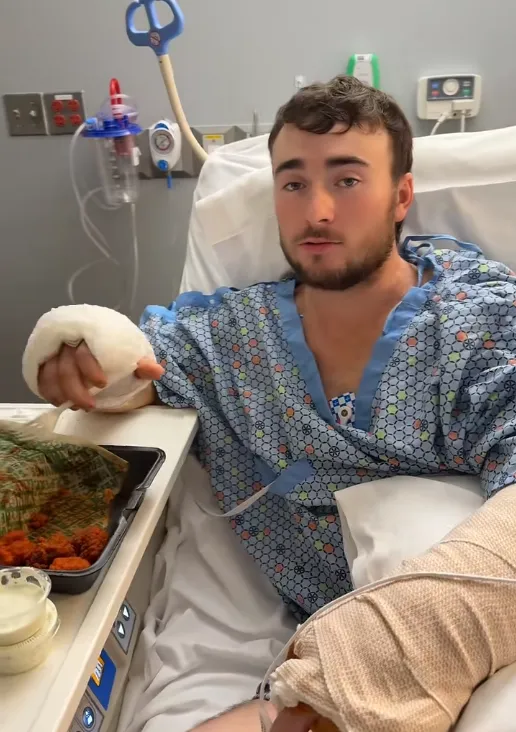
It resembles escalation.
Escalation to contain spread. Escalation to preserve what can still be saved. Escalation to prevent systemic collapse.
The days ahead are likely to involve careful reassessment — possibly additional procedures, possibly revised treatment strategies. Complex surgical recoveries often reveal their full scope only in stages. Each stage demands recalibration.
The window to stabilize may feel smaller now. But it is not necessarily closed.
And as hard as the update was to hear, it also means one thing clearly: the severity is now fully acknowledged. There are no illusions left. Only decisions.
For the family, the waiting continues — heavier this time.
For the medical team, the mission is unchanged: stop the spread, protect circulation, support systemic stability.
For supporters watching from afar, the shock lingers.
Because a procedure meant to relieve pressure instead exposed a deeper crisis.
And now, the fight has entered a more critical phase — one where every hour matters.